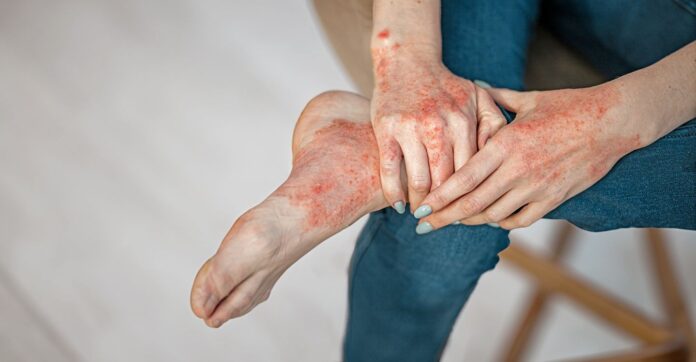
Eczema is not merely a cosmetic concern; it is a chronic inflammatory condition that fundamentally alters how the skin functions. For those living with it, the daily struggle isn’t just about redness or dryness—it is about managing a compromised skin barrier that fails to retain moisture and protect against irritants.
While there is no universal cure, a strategic, consistent skincare routine can significantly reduce flare-ups and prevent complications. The key lies in understanding the mechanics of the skin and avoiding common pitfalls that worsen inflammation.
The Core Challenge: Breaking the Itch-Scratch Cycle
The most critical aspect of eczema management is controlling the urge to scratch. According to Dr. Jessica Wu, a dermatologist in Los Angeles, itching is often the first sign of an outbreak.
“The scratching stimulates nerve endings in the skin and causes inflammation in the area, which turns into a visible rash and triggers further itching,” explains Dr. Wu.
This creates a vicious cycle: Itch → Scratch → Inflammation → Rash → More Itch.
Breaking this cycle is essential not only for comfort but for safety. Scratching damages the skin’s protective layer, creating entry points for bacteria. Dr. Wu notes a rising trend in patients suffering from secondary infections, particularly from Staphylococcus aureus, which can enter through open sores caused by scratching. Controlling the itch is therefore the primary defense against both visible rashes and serious skin infections.
High-Risk Zones: Face, Hands, and Body
Eczema does not affect all skin equally. Its impact varies significantly by location due to differences in skin thickness and exposure.
Facial Sensitivity
The skin on the face is thinner and more sensitive than elsewhere. This makes it highly susceptible to contact eczema, often triggered by cosmetics or skincare products. Common areas for flare-ups include:
* Eyelids: Leading to red, swollen, and flaky skin.
* Around the mouth: Often irritated by food or saliva.
Because facial eczema is highly visible, early intervention is crucial to prevent long-term discoloration or thickening of the skin.
Hand Vulnerability
Hands are among the most frequently affected areas, largely due to environmental exposure. Frequent hand-washing, while necessary for hygiene, strips natural oils and weakens the skin barrier.
* The Risk: Cracked skin from dryness invites infection.
* The Solution: Avoid alcohol-based hand sanitizers, especially those containing methanol, which can be severely irritating. Opt for gentle, soap-free cleansers with water. If sanitizer is unavoidable, choose a mild formula and moisturize immediately after use.
Body Changes
On the body, chronic scratching can lead to lichenification —a thickening and darkening of the skin. This discoloration can persist for months even after the itching subsides, highlighting the importance of early and consistent treatment.
Building a Safe Skincare Routine
A successful eczema routine rests on two pillars: Hydration and Soothing. The goal is to repair the skin barrier without introducing new irritants.
Ingredients to Embrace
- Hyaluronic Acid: This ingredient holds moisture effectively without causing irritation. Research suggests it helps regulate the immune response in atopic dermatitis, though it works best as part of a broader treatment plan rather than a standalone cure.
- Fragrance-Free Products: Always choose products labeled “fragrance-free.” Avoid “unscented” items, which may contain masking fragrances that can still trigger reactions.
- Gentle Cleansers: Use non-soap, hydrating washes that clean without stripping the skin barrier.
Ingredients to Avoid
Certain popular skincare ingredients can exacerbate eczema symptoms:
* Retinol: While beneficial for anti-aging, it can trigger flares in sensitive skin.
* Alpha Hydroxy Acids (AHAs) and Salicylic Acid: These exfoliants can be too harsh for compromised skin.
* Lanolin and Fragrances: Known aggravators that should be strictly avoided.
The Role of Makeup
Makeup is not off-limits, but caution is required. Dr. Joshua Zeichner, a dermatologist at Mount Sinai Hospital, advises sticking to fragrance-free cosmetics. When removing makeup, avoid traditional wipes, which can be abrasive. Instead, use a biphasic or oil-based remover to gently dissolve products without friction.
Medication Management: Less Can Be More
Over-the-counter corticosteroids are effective for reducing inflammation, but they carry risks if misused. Long-term or excessive use can cause skin thinning, particularly in sensitive areas like the face, underarms, and groin.
- Follow Professional Guidance: Dermatologists often recommend a “weekend therapy” approach—using topical steroids only two days a week between flares, while relying on moisturizer on other days.
- Adhere to Instructions: Never apply strong steroids to thin-skinned areas unless explicitly directed by a doctor.
A Daily Routine Framework
Every individual’s skin is unique, so personalized advice from a dermatologist is essential. However, a general framework can serve as a starting point:
Morning Routine
- Cleanse: If you have oily skin, use a gentle, hydrating cleanser. For dry or normal skin, splashing with water or using a mild, soap-free cleanser is sufficient.
- Treat: Apply any prescribed topical medications.
- Protect: Finish with a broad-spectrum sunscreen (SPF 30 or higher). Sun protection prevents further skin damage and irritation.
Evening Routine
- Cleanse: Wash with a gentle cleanser or water. If wearing makeup, use a non-irritating oil-based remover.
- Treat: Apply prescription creams or corticosteroids as directed.
- Moisturize: Apply moisturizer within five minutes of bathing or washing to lock in hydration. This timing is critical for maximizing moisture retention.
- Environment: Consider using a cool-mist humidifier in the bedroom to prevent dry air from dehydrating the skin overnight.
Adapting to Aging Skin
Eczema symptoms and skin needs evolve over time. As skin ages, it naturally becomes drier and thinner, which can alter how eczema presents itself. Regular check-ins with a dermatologist ensure that your routine adapts to these changes, incorporating newer treatments and adjusting product choices to maintain skin health.
Conclusion
Managing eczema requires a shift from reactive treatment to proactive maintenance. By focusing on hydration, avoiding known irritants, and strictly controlling the itch-scratch cycle, individuals can significantly improve their quality of life. A disciplined, dermatologist-approved routine—combining gentle cleansing, strategic moisturizing, and careful medication use—remains the most effective tool for keeping eczema symptoms in check.